Grade 1 · Liposuction Only
- Lowest cost option
- Minimal incisions (3-4mm)
- Near-invisible scarring
- Fastest recovery
- Only addresses fat
- Doesn't remove glandular tissue
- Recurrence risk if gland present
- Requires Grade 1 anatomy
Grade-based male breast reduction in Seomyeon, Busan. Liposuction, glandular excision, or combination — chosen based on your grade. Transparent USD/KRW pricing from $1,111. Personally performed by Dr. Moon Hyeon-chang — 800+ gynecomastia procedures over 15 years at our Busan Seomyeon clinic.


Before booking gynecomastia surgery in Busan, learn from Dr. Moon Hyeon-chang about the grade-based approach at our Seomyeon clinic. 15+ years of experience, 800+ male breast reduction procedures, all explained in clear English.
Dr. Moon personally performs every gynecomastia surgery at our Busan Seomyeon practice. Accurate grading is critical — Grade 1 patients don't need excision, Grade 4 needs skin tightening. Wrong technique = poor outcome.

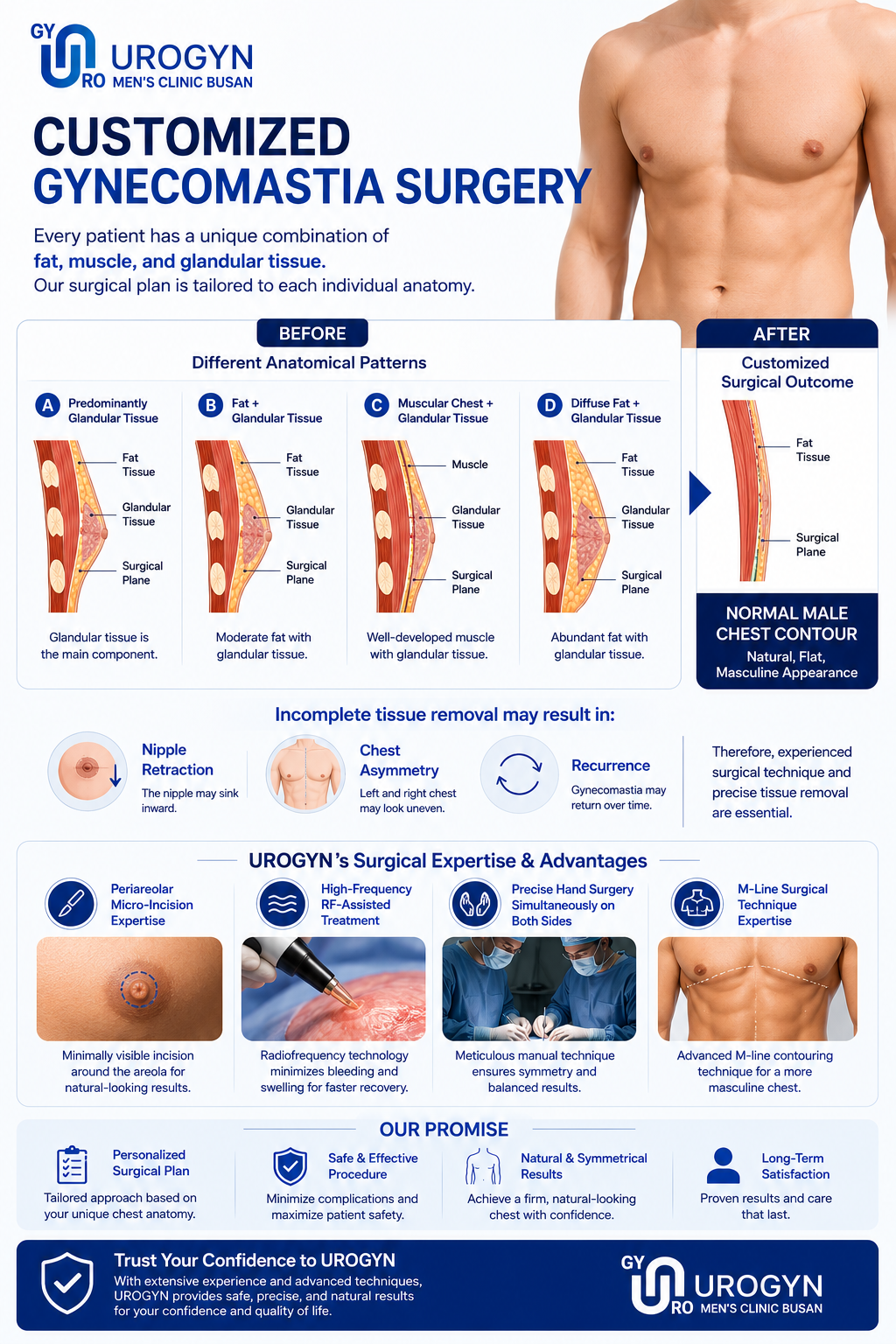
Most patients return to desk work within 5–7 days. Compression garment worn for 4–6 weeks. Final result visible at 3 months.
No filter. Each technique addresses different gynecomastia grades. The wrong choice produces poor results — accurate grading by Dr. Moon at our Busan Seomyeon clinic determines the right approach.
| Liposuction Only | Liposuction + Excision | Excision + Skin | |
|---|---|---|---|
| Price (USD) | $1,111 | $2,222 | $3,704 |
| Price (KRW) | ₩1.5M | ₩3M | ₩5M |
| Best for grade | Grade 1 (fat only) | Grade 2-3 (mixed) | Grade 4 (with skin excess) |
| Procedure time | 60–90 min | 90–120 min | 120 min+ |
| Anesthesia | Local + sedation | Local + sedation | General |
| Incision | 3-4mm punctures | Areolar 1-2cm | Areolar + skin pattern |
| Glandular removal | × No | ✓ Yes | ✓ Yes + skin |
| Compression garment | 4 weeks | 4–6 weeks | 6 weeks |
| Return to work | 3–5 days | 5–7 days | 7–10 days |
| Full recovery | 4 weeks | 4–6 weeks | 6–8 weeks |
| Scarring | Near-invisible | Faint areolar line | Visible (hidden by clothing) |
| Risk of recurrence | ~ If gland present | ✓ Minimal | ✓ Minimal |
| Stay in Korea | ✓ 3–5 days | ✓ 5–7 days | ✓ 7–10 days |
Three surgical approaches at our Busan Seomyeon clinic — each for different gynecomastia grades. Written by Dr. Moon for international patients deciding which technique fits their anatomy.
Three quick questions. Anonymous. We'll suggest the likely technique based on your symptoms and grade. Final recommendation requires Dr. Moon's physical examination and grading.
Get a tailored recommendation based on your chest tissue type, severity, and goals.
Realistic outcome expectations per technique. Korean medical advertising law restricts public posting of identifiable patient photos at our Busan Seomyeon clinic.
At 1 week post-procedure, swelling is 60% resolved. Bruising visible but fading. Most patients return to desk work. Compression garment worn 23 hours/day. Photo update to Dr. Moon for healing check.
At 3 months, final cosmetic result visible. Areolar scarring barely visible (Grade 2-3) or near-invisible (Grade 1 lipo). Final flat chest achieved. Compression garment discontinued. End of standard follow-up period.
The exact 60-120 minute procedure at our Seomyeon, Busan clinic — from grading examination to walking out.
Physical examination of chest tissue. Identification of fat vs glandular tissue. Skin elasticity assessment. Photographic documentation (medical record only). Grade determination (1-4).
Hormone panel (testosterone, estradiol, LH, prolactin) to rule out endocrine causes. ECG if over 40. Photo documentation. Consent forms signed in English. Markings made before procedure.
Local anesthesia + IV sedation (Grade 1-3) or general anesthesia (Grade 4). Liposuction through 3-4mm punctures, gland excision through areolar incision if indicated. Dr. Moon personally performs every step.
Compression garment applied (provided). English aftercare instructions. Antibiotics and pain medication prescribed. WhatsApp to Dr. Moon activated. Same-day discharge to hotel.
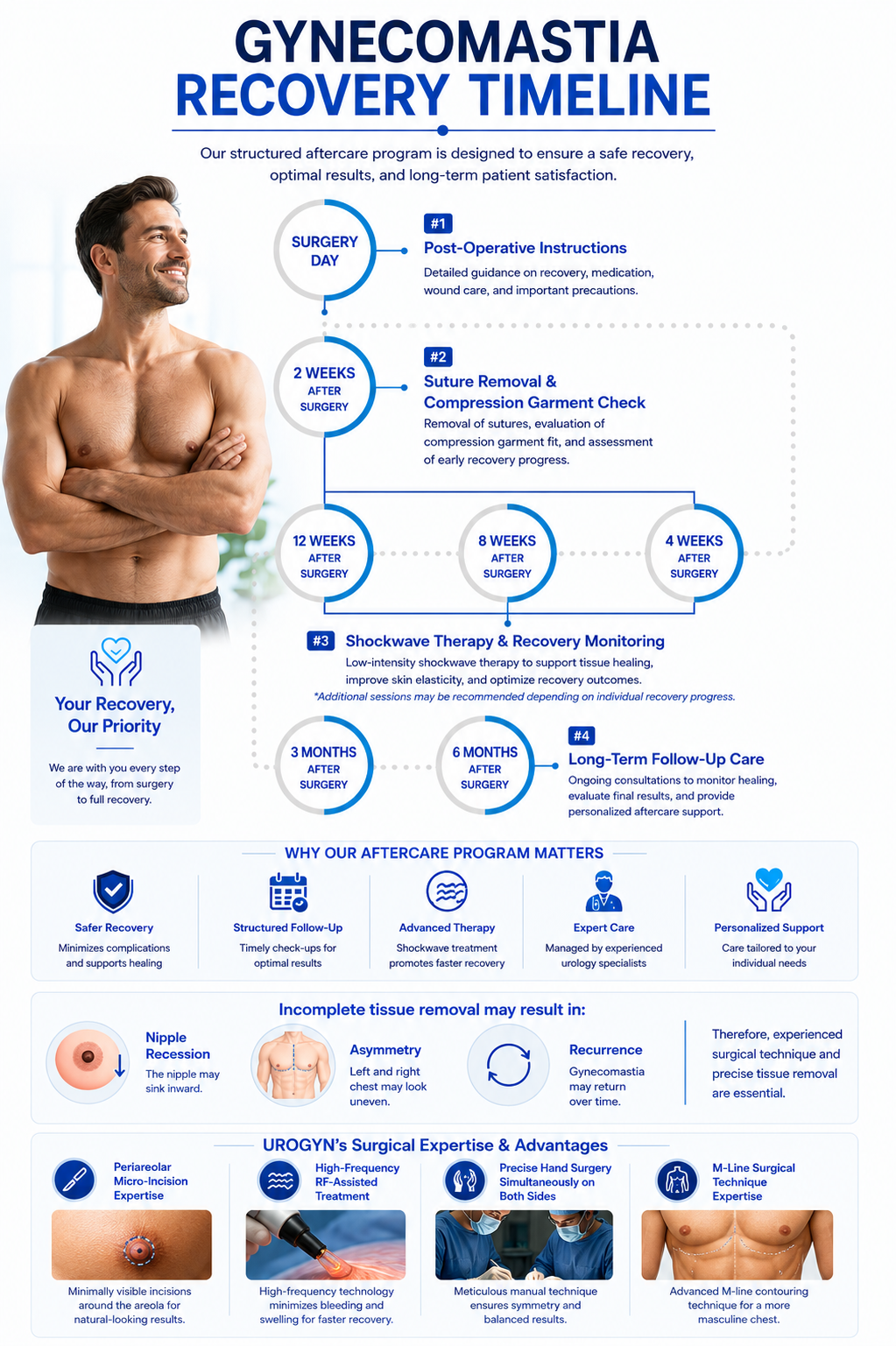
Realistic recovery timeline for gynecomastia surgery. Most international patients fly home Day 5-7, wear compression garment for 4-6 weeks, and see final result at 3 months.
Compression garment on (worn 23 hours/day). Mild swelling and bruising normal. Pain controlled with prescribed medication. Sleep on back recommended. Walk out of clinic same day.
Swelling peaks then decreases. Bruising visible (chest, sometimes abdomen). Light walking encouraged. Compression garment continuous. Most Grade 1 patients fly home Day 3-5.
Most patients return to desk work. Bruising fading. Swelling 60% resolved. WhatsApp Dr. Moon photo for healing check. Grade 2-4 patients fly home this week.
Compression worn 23 hours daily. Light exercise OK (walking, stationary bike). Avoid chest exercises, swimming, hot tubs. Bruising mostly resolved.
Compression worn 12 hours/day (or as Dr. Moon advises). All activities resume gradually. Final swelling resolving. Photo update to Dr. Moon. Grade 1: full healing. Grade 2-3: 80% result visible.
Final cosmetic result visible. Scars maturing (areolar barely visible). Photo to Dr. Moon for records. Final flat chest achieved. End of standard follow-up period.
Most cosmetic surgery clinics don't talk about complications. We do at Urogyn Busan Seomyeon. Honest numbers from 800+ procedures.
Gynecomastia surgery has low complication rates when performed by experienced surgeons with accurate grading. Below is what 15 years of practice and 800+ procedures have taught us about realistic rates at Urogyn Busan.
Two international patients share their experience flying to Busan, Seomyeon for gynecomastia surgery — grading, procedure, and 6-month results.

"Grade 1 — pure fat, no gland. Liposuction in Busan, $1,200 total. Compression garment 4 weeks. Flat chest at 3 months. Wish I'd done this in my 20s."
"Grade 3 — both fat and gland. Combined surgery in Busan, much cheaper than Germany. 6 months later, completely flat. Confident at the beach again."
Pinch your chest tissue between fingers. Pure soft fat = Grade 1. Firm disc behind nipple = Grade 2-3 (glandular component). Significantly loose/saggy skin = Grade 4. Final grading requires Dr. Moon's physical examination. Send WhatsApp photos for preliminary grading.
Properly performed surgery has under 2% recurrence. Lipo-only on Grade 2-3 (when glandular tissue is present) has 15-20% recurrence because the disc is left behind. Accurate grading and appropriate technique prevent this. Weight maintenance important — significant weight gain can re-deposit fat.
If you're significantly overweight, weight loss first is recommended. Some gynecomastia resolves with weight loss alone (Grade 1 'pseudogynecomastia'). For glandular gynecomastia (Grade 2-4), weight loss helps but doesn't eliminate the firm tissue — surgery still needed. Within 10-15kg of goal weight is ideal pre-surgery.
Three main causes: (1) Hormonal — testosterone/estrogen imbalance during puberty or aging. (2) Medication-induced — anabolic steroids, antidepressants, some BP meds. (3) Idiopathic — no clear cause. Dr. Moon screens for endocrine causes before surgery — sometimes addressing the cause (e.g., stopping steroids) is the right first step.
Continuous 23-hour wear for first 2 weeks. Then 12-16 hours/day for weeks 3-6. Total: 4-6 weeks. Garment minimizes swelling, prevents seroma, helps skin retract. Quality medical compression garment provided post-surgery.
Grade 1 (liposuction only): 3-4mm punctures, near-invisible at 3 months. Grade 2-3 (areolar excision): faint horizontal line at areolar border, very well-hidden. Grade 4 (skin excision): planned visible scars hidden by clothing/swim shorts.
Walking: same day. Stationary bike: Week 1. Light cardio: Week 2-3. Chest exercises (push-ups, bench press): Week 6+. Heavy lifting: Week 8+. Following this timeline minimizes recurrence risk.
Yes, common combinations: Gynecomastia + Vasectomy (same visit). Gynecomastia + Liposuction of flanks/abdomen (additional cost). Gynecomastia + Hair transplant (different day). Total stay typically 7-10 days for combinations.
Most insurance considers gynecomastia 'cosmetic' and doesn't cover. Exception: documented physical/psychological symptoms (back pain, depression, social anxiety) sometimes covered. Itemized English receipts available for reimbursement attempts. Most international patients pay out-of-pocket.
Credit card, bank transfer, or crypto accepted. Card descriptor reads "Busan Health Clinic" — not the procedure name. Payment: 50% deposit / 50% on procedure day. Itemized receipts in English available.
Korean pricing reflects lower facility costs, no insurance markup, direct-pay model. Gynecomastia at Urogyn Busan ($1,111-$3,704) costs 60-80% less than US gynecomastia surgery ($5,000-$10,000). Same techniques, KFDA-approved equipment, equivalent or higher surgical volume.
Three reasons: (1) 25-35% lower cost for identical procedure, (2) Dr. Moon performs every consultation and surgery personally (800+ gynecomastia), (3) Seomyeon medical district has English-speaking staff and easy hotel access. Discreet, professional care.
Often combined with gynecomastia surgery. Reduces enlarged or projecting nipples. Outpatient, minimal recovery. From $370.
Read moreReduces enlarged areola. Common adjunct to gynecomastia surgery for complete aesthetic result. From $370.
Read moreLiposuction of pubic area. Often combined with gynecomastia for comprehensive body contouring. From $741.
Read moreFree, no commitment. Send WhatsApp photos of your chest — Dr. Moon will grade your gynecomastia, recommend the right technique, and quote your total cost for visiting our Seomyeon, Busan clinic — from $1,111 Liposuction to $3,704 premium combined surgery.

Address:
7F-702, Ion City Building, 74 Seomyeon-ro, Busanjin-gu, Busan, South Korea
All Rights Reserved | Urogyn Men's Clinic Busan